Diverticular disease and other colitis
Diverticular disease:
What is Diverticular disease:
Diverticular disease encompasses two conditions “diverticulosis” and “diverticulitis”. The term “diverticulum” has a latin origin, describing a “wayside house of ill repute”. Diverticulosis is a formation of blind outpouchings from the wall of the large bowel. They can effect the entire colon but are most common in the lower portion of the colon (sigmoid colon). Diverticulitis is the inflammation of the diverticulum.
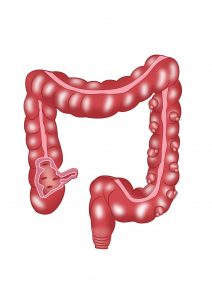
Diverticular disease of the colon. It can occur throughout the colon, but is typically symptomatic on the left side.
Who is at risk:
Diverticular disease is common in patient having a “western diet” (high amounts of processed foods and low volumes of fiber). This precipitates constipation and therefore high pressure within the colon that in tern may result in formations of the blind outpouchings. Diverticular disease has been associated with several factors in population studies including:
- Aging (50% of 50 year olds, and 70% of 70 year olds.)
- Obesity
- Sedentary lifestyle
- Diet low in fiber and high in animal fat
Consumption of seeds, beans and nuts in moderation has not been demonstrated to precipitate symptoms of diverticulitis. In fact, there is a publication demonstrating that regular consumption of popcorn may have a protective effect.
What are the symptoms of Diverticular disease:
The majority of patients with Diverticular disease will not have any symptoms or complications of the conditions and may live their whole life without being aware of its presence. Common symptoms of Diverticular disease may include:
- Fever
- Nausea, vomiting or feeling bloated
- Change of bowel habit (diarrhea or constipation)
- Bright blood per rectum
However, symptoms of Diverticular disease are not specific to this condition. It may be of benefit to be aware of complications of Diverticular disease to understand the acuity of symptoms.
A small percentage of patients may develop complications that are described below:
- Diverticular Bleeding: This is an episode of bright red, painless bleeding. The volume may be significant (a cupful). Commonly a blood vessel runs within the diverticulum, and if that vessel is torn, bleeding ensures. This condition is not associated with inflammation and is therefore painless. An alternative diagnosis needs to be thought in patients who present with painful bleeding, even in the presence of known Diverticular disease.
- Acute Diverticulitis: This is inflammation of a diverticulum that is due to a microscopic perforation of the diverticulum. It is an acute condition that is associated with systemic symptoms (fevers, sweats, malaise) and local signs of colonic inflammation (abdominal pain and tenderness on palpation). Patients with severe acute diverticulitis can be systemically unwell and require urgent surgery and intensive care support.
- Diverticular abscess: In some cases of acute diverticulitis an area of inflammation forms a pocket of pus termed an abscess.
- Diverticular fistula: A fistula is a communication between a hollow organ (bowel) and another surface. The most common sites of a diverticular fistula are to the:
- Bladder: “Colovesical fistula”
patients may notice gas or stool when urinating - Vagina: “Colovaginal fistula”
patients may have faecal discharge per vagina - Skin: “Colocutaneous fistula”
Recurrent discharge of pus or stool from a defect in the skin, commonly at site of previous drain
- Bladder: “Colovesical fistula”
- Diverticular stricture: An area of diverticulitis can form a scar that narrows the bowel over a period of time. This narrowing of the bowel is called a stricture. Sometimes the stricture can cause a complete large bowel obstruction (a bowel blockage). Patients that are unable to pass bowel motion and gas may have an acute large bowel obstruction and may require an urgent operation to fix this.
- Smouldering Diverticulitis: Some patients suffer from recurrent attacks of diverticulitis that require frequent admissions to hospital and multiple courses of antibiotics and long-term pain killers.
How is Diverticular disease diagnosed:
Diverticular disease can be seen during colonoscopy, X-ray contrast enema or a CAT scan. Since Diverticular disease is so prevalent, it is essential to confirm that the cause of the patient’s symptoms are due to Diverticular disease. A colonoscopy following resolution of an acute attack of diverticulitis is sometimes required to exclude more sinister bowel pathology like colorectal cancer.
What is the treatment of Diverticular disease:
Eating a diverse diet, having regular bowel movements whilst avoiding constipation and straining can reduce complications of Diverticular disease. A referral to a dietician may assist with this. A daily intake of 20-35grams of fibre is recommended for healthy bowel function. An over-the-counter fibre supplement, such as psyllium husk, may assist with this. Increasing fibre intake should be gradual (increase by 5grams every 1-2weeks), as this may be associated with increased bloating and flatulence.
Treatment of complications of Diverticular disease depend on the specific condition:
- Diverticular bleeding: Most bleeds are self limiting, but may require blood transfusion and supportive care. CT arterial imaging at the time of the bleed may identify the offending vessel, and when seen, the vessel can be occluded using interventional radiological techniques. Colonoscopy may be required for persistent bleeding and the colonoscopist can clip the bleeding diverticulum if it is seen. The decision to proceed with intervention is complex due to the risk of complications.
- Acute Diverticulitis: Treatment of this is a spectrum that depends on the severity of the attack. Inflammation may be mild, and can subside with several days of over the counter pain killers, moderate, requiring admission to hospital and intravenous antibiotics, or severe, requiring urgent surgery, bowel resection and at times a stoma (where bowel is brought to the surface of the abdomen and a bag collects the stool). In patients who require a stoma, this can be reversed in over 95% of patients that chose to undergo further surgery in 3-6month. Typically, the first attack of diverticulitis is the worst, and it is unlikely for patients to require urgent surgery and stoma for recurrent attacks. A specialised colorectal surgeon is more likely to be able to perform this surgery laparoscopically (keyhole) and avoid the need for a stoma.
- Diverticular abscess: Depending on the size of the abscess, a drain may be required to drain the pus, because antibiotics typically cannot get to the centre of the abscess. The drain is placed under X-ray guidance in the radiology department and may remain for a number of days.
- Diverticular fistula: These fistulas are unlikely to resolve without surgery. A resection of the offending bowel is required (usually sigmoid colon). Sometimes a temporary stoma is required (for 3-6months). A specialist colorectal surgeon may perform this laparoscopically (keyhole).
- Diverticular stricture: This requires a major surgical resection and may require a temporary stoma). In experienced hands this can be performed laparoscopically (keyhole).
- Smouldering Diverticulitis: Whilst development of a life-threatening attack of diverticulitis with recurrent attacks is unlikely, some patients benefit from a surgical resection of the offending area of bowel as a lifestyle choice. The threshold for resection depends on the age of the patient, frequency of attacks and number of co-morbidities (anaesthetic risks). More than 2-3 attacks in a calendar year is grounds for discussion for most patients.
Radiation, Microscopic and Ischaemic:
- Radiation colitis – Radiotherapy as treatment of cancers can be delivered as external beam (like performing an X-Ray) or by brachytherapy (placement of radioactive beads inside the body). Radiation injury to the bowel occurs when the bowel is in the line of the irradiated field. Such injuries can be acute (within 6 month of radiation) or chronic (6-12 months, but can be delayed for decades). The damage of the bowel lining caused by radiation causes diarrhea, while the damage to the small vessels that supply the bowel can reduced blood flow and scarring. Treatment of radiation injuries can be medical, endoscopic (using a colonoscope) or surgical. The treatment should be tailored to the individual and the specific injury. Assessmnet of injury may require CT, MRI and/or colonoscopy.
- Microscopic colitis (MC) is an inflammation of the large bowel and is a relative common cause of non-bloody diarrhea. The exact cause of MC is not know. Diagnosis is confirmed by biopsy at time of colonoscopy and can be classified as: minimal change, lymphocytic or collagenous colitis. Treatment is usually medical and the role of surgery is limited to rare cases.
- Ischaemic colitis is a condition that is associated with a transient inadequate blood supply, most commonly to the part of the colon which lies near the spleen. Patients typically present with abdominal pain (more common on the left) and rectal bleeding. It is a condition that effects older adults with a history of cardiovascular disease. Silent ischaemia (small heart attack) is not infrequently associated with an acute attack.
In the acute setting the condition is typically self-limiting and rarely requires surgical intervention. Chronic stricture (narrowing of the colon) can develop following an acute attack, as such a colonoscopy is frequently arranged as follow up to exclude complications and confirm the original diagnosis.

